Introduction
Rabies is one of the oldest and most feared zoonotic diseases known to humanity. It is an acute, progressive, and nearly always fatal infection of the central nervous system (CNS) caused by the rabies virus. Affecting both animals and humans, it poses a significant threat to veterinary and public health worldwide. Without rapid intervention, rabies leads to encephalitis, severe neurological dysfunction, and ultimately death. Its impact underscores the importance of vaccination and early post-exposure prophylaxis, which remain the only life-saving measures against the disease.
Causative Agent and Classification
- Family: Rhabdoviridae
- Genus: Lyssavirus
- Species: Rabies lyssavirus
The name Lyssa comes from the Greek word meaning “madness” or “rage,” reflecting the classical furious form of the disease. Although there are several lyssaviruses, rabies virus is the primary cause of rabies in domestic and wild animals.
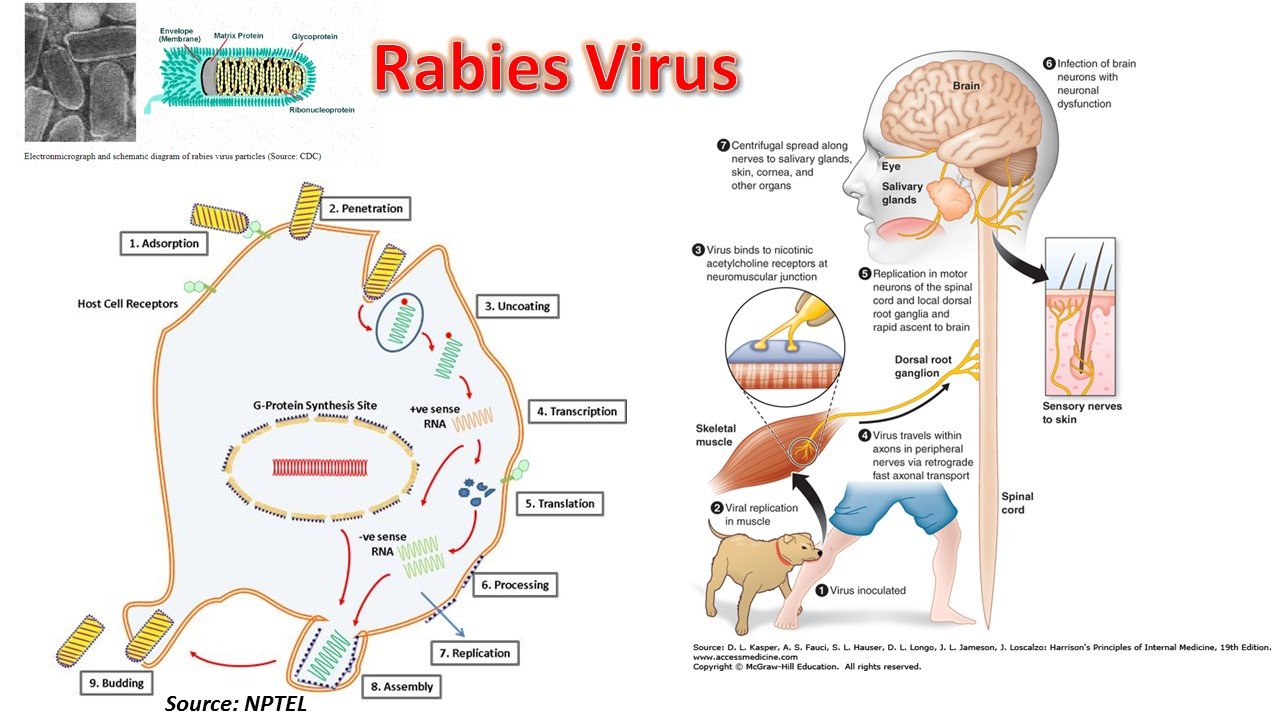
Morphology of Rabies Virus
- Shape: Bullet-shaped viral particle
- Size: ~75 × 180 nm
- Nucleic acid: Single-stranded negative-sense RNA genome
- Proteins: Encodes five structural proteins – G (glycoprotein), M (matrix), N (nucleoprotein), L (polymerase), and P (phosphoprotein).
- Envelope: Surrounded by a lipid envelope with glycoprotein spikes, which are essential for host cell entry and immunogenicity.
This unique morphology allows the virus to evade immune defenses during neuronal transport and to maintain infectivity in diverse environments.
Resistance
- Stable at cold temperatures and in decaying carcasses (infective for weeks).
- Sensitive to lipid solvents (alcohol, ether, chloroform).
- Inactivated by heat (50 °C for 1 hour, 60 °C for 5 minutes), ultraviolet light, and common disinfectants (formalin, phenol, betapropiolactone).
Transmission and Pathogenesis
Rabies is transmitted almost exclusively through the saliva of an infected animal, most commonly via bites. The principal reservoirs include dogs, cats, foxes, jackals, and bats.
Pathogenesis:
- Virus enters through bite wounds and replicates in muscle cells near the inoculation site.
- It gains access to peripheral nerves and travels retrogradely toward the CNS.
- Once in the CNS, the virus replicates extensively, leading to encephalomyelitis.
- From the brain, the virus spreads centrifugally to salivary glands, heart, adrenal glands, and skin.
Because the virus travels within nerve axons, it is protected from immune surveillance, which explains the delay before antibody response and the high lethality once CNS infection is established.
Clinical Signs
Two main clinical forms exist:
- Furious Rabies: Restlessness, aggression, excessive salivation, difficulty swallowing (hydrophobia), seizures, paralysis, and death due to respiratory or cardiac failure.
- Paralytic (“Dumb”) Rabies: Lethargy, progressive paralysis, drooping jaw, loss of voice, inability to swallow, eventually leading to death.
Incubation period: 20–90 days (shorter if the bite is close to the head or if the viral dose is high).
Diagnosis
Diagnosis is crucial both for animal control and human exposure management.
- Histopathology: Detection of Negri bodies (eosinophilic cytoplasmic inclusions) in neurons of the hippocampus or Purkinje cells.
- Direct Fluorescent Antibody Test (dFAT): Gold standard for detecting viral antigens in brain tissue.
- PCR & Molecular Testing: Detects viral RNA in saliva, skin biopsies, or CSF.
- Virus Isolation: In cell culture or laboratory animals (less commonly used now).
Treatment
Once clinical signs of rabies appear, treatment is not effective. Supportive therapy cannot stop progression to death. Therefore, prevention through vaccination is the cornerstone of rabies control.
Prevention and Vaccination
Post-Exposure Prophylaxis (PEP) in Humans and Animals:
- Immediate wound cleansing with soap and water.
- Passive immunization: Rabies immunoglobulin (in humans) infiltrated around the wound.
- Active immunization: Multiple doses of modern cell-culture vaccines.
Pre-Exposure Prophylaxis:
Recommended for veterinarians, laboratory workers, animal handlers, and populations in rabies-endemic regions.
Animal Vaccination:
- Regular rabies vaccination in dogs, cats, and livestock is essential for breaking the transmission cycle.
- Mass dog vaccination programs have been proven to drastically reduce rabies cases globally.
Public Health and Veterinary Importance
Rabies remains endemic in many parts of Africa, Asia, and developing regions. Because it is a 100% preventable disease, early recognition and preventive veterinary care are essential. Vaccinating pets not only saves animal lives but also protects families and communities from this fatal zoonosis.
Our Clinical Commitment
At Dr. Boudi Widad Veterinary Clinic, we strongly emphasize the importance of rabies prevention. We provide:
- Immediate wound management in suspected bite cases.
- Rabies vaccination for dogs, cats, and livestock to ensure herd immunity.
- Post-exposure prophylaxis guidance and follow-up for both animals and pet owners.
By choosing timely vaccination and veterinary care, rabies can be completely prevented. Protect your pets, protect yourself, and protect your community.
